Hi Steve,
I am planning the second Celebration of Life for families with special needs kids in NH – by invitation right now to see how it goes and I came upon my letter to a young woman whose non-profit helped me put on Maddie’s Celebration last year. I have copied it and hope you can use it some way. Maddie has VACTERL. Keeping in mind the letter was from last year, to date, Maddie still struggles with eating, and GI issues, but many other health related issues have been kept at bay. I often tell people, when they with good will say how well she looks, that we have to force health on her. Every single minute of every day we have to watch our Maddie because infection could strike anywhere, or question has she eaten, had enough fluid, does she need a rest and so on. She is our little happy beauty and I can’t imagine life without our sweet girl.
“Dear ***, Thank you for you phone call. It made my day, my Christmas. I wanted to tell you that when I saw on the MSN news feed about how a young woman was helping people by fulfilling dreams, how inspired and filled with hope I was for my daughter Maddie. I was drawn in immediately because you have VATER or VACTERL association as does Maddie. I suddenly saw my little girl grown up and having a full life helping others and I thought, I would love to have you in Maddie’s life as a role model and hear your journey through life with this difficult, at times painful and often misunderstood condition.
While I am writing this, my little girl is lying on the couch, we spent the morning at Dartmouth to fix her tube since her flush wasn’t working last night, and the doctor put silver nitrate on irritated tissue under her Ce-colostomy tube. She is having a sick spell right now that has already lasted a week and a half. You know exactly what I am talking about.
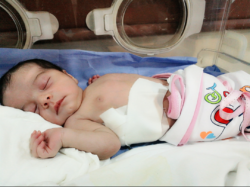
Madeline Lucy was Dan’s and my four child and first girl. We kept the gender a surprise and I was overjoyed when, on February 1rst, 2009, Dan looked at me and said, “It’s a girl!” I still remember her on my chest and I was crying saying “I can’t believe it!” I knew God had a wondrous plan for the baby, because a week before she was born I had a vision – I was resting in my room and I suddenly woke up and saw the bedroom window filled with a beautiful soft light and a breeze was blowing the sheer curtains over the bassinet that I had set up for the baby. I suddenly knew, the baby was going to be Madeline Lucy. Her name means Tower of Light.
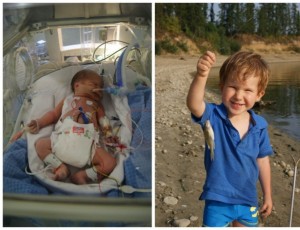
We noticed very quickly that something was wrong, but didn’t understand the severity as it was to all come in the days, weeks and now years to follow. Twenty-four hours after Maddie was born she was taken to Dartmouth Hitchcock in Lebanon, New Hampshire, because of finding a hole in her heart, then two days after that to Boston Children’s Hospital, because another hole was found. There she had open heart surgery to repair three holes in her heart. While I knew it was serious I did not understand the full extend of what was happening as my mind and my body had shut down. I was heart broken and physically ill for fear that my baby was going to die and I did not know how to handle this, death is not new to my family. My parents drove from Ontario, Canada to be with Dan and me, and Dan’s brother was with us in Boston. They knew that Maddie might not make it and didn’t tell me that the doctors had uncovered the third hole in her heart. After her surgery they all breathed a sigh of relief then explained the extent of the situation to me. My parents had to go back home after a few days and thanks to some tough love words from my mother, I had pulled myself together. The night before they left for Canada, my Mom and Dad were crying, because I was lying in the hotel bed sobbing, but my mom said, “Liza, please, you have to pull yourself together, that baby needs you, Dan needs you. I can’t leave you like this.” Sometimes you need a hug and other times a good shake and they were right, when I wasn’t near Maddie, her little heart would slow down, her oxygen would drop, but when I was close by kissing and holding her little hands, her heart would beat faster and her oxygen levels would improve. It was truly amazing.
My sister-in-law, was back in our home in New Hampshire, 2 1/2 hours away looking after my three little boys, the oldest only five and half at the time. She was having them stay with different family and friends, meals were coming in, then Dan’s parents came from Kentucky and stayed for three weeks. It is an ordeal to orchestrate someone else’s family when they are away for two months with a sick child.
One night when we came home to visit the boys, we got a call that Maddie had flat lined from choking on some milk, but was quickly revived. We rushed back to Boston and that day they discovered the Tracheal-Esophageal fistula. Dan and I had continuously questioned why she kept choking and this was the initial reason why I sent her to the nursery that first night of her birth. Follow your instincts and question everything, no matter how trivial it may seem at the time.
After her throat surgery Maddie was on a feeding tube, then a few weeks later was brought back to Dartmouth, so that I could be mother to my boys and my baby in the hospital. I could not stand being away from my boys, but I needed to be with Maddie. It was pure agony, but after eight weeks of being in the hospital Maddie came home. She had a special feeding bottle but after not nursing for nearly two and half months Maddie was full time nursing at three months and that was pure delight for me and her.
Three months after her birth she had her third surgery, which was to repair her anal fistula. This was very traumatizing, because of the long painful process after the surgery to expand the new anal opening. Maddie was on antibiotics to prevent kidney infections so her bottom skin would break down and bleed, she could not pass stool without medications, enema’s and suppositories. These were painful for her and I often felt like I was torturing my own child and felt helpless. We landed in the ER several times for kidney infections and blockage. She had a Ce-colostomy surgery this past summer and still has issues and will be going to Boston for them to look at her and give their opinion of how to help her. The surgery for the c-tube was difficult for Maddie to recover from, she spent the night vomiting and having diarrhea every twenty minutes and she was in horrible pain. I was wondering what kind of mistake I had made, but fortunately it got better. She does not have an appetite and nibbles like a little mouse on food and we often supplement with Instant Carnation breakfast, Ensure or yogurt drinks just to make sure she has nourishment. These are Maddie’s biggest struggles.
Winter 2009, Maddie had two hand surgeries in Boston; her left hand has four fingers as the thumb didn’t work, so they moved her pointer finger and made that her thumb. With the right hand they warned me that they might not be able to save the thumb, but I burst into tears and I was quickly consoled that they would do everything to save her other hand, which they did. I love her little hands and Nickle Creek has a beautiful song called “The Hand Song”, by Nickle Creek, that I sing to Maddie sometimes.
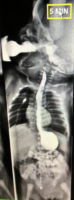
At this point my dates get fuzzy, because our life became a whirlwind of trials; Dan lost his job, I began work as an LNA, and became pregnant with our fifth child. Dan is now teaching at a small Catholic school and am I home again. Maddie in the meantime was to have Kidney Reflux, Tethered Cord Spinal surgery, and again her latest surgery was for the Ce-costomy. While at times it is difficult to have two other babies in tow, my two youngest, both girls have been a comfort to Maddie. She loves her Sisters.
There was a time when Maddie was about two and a half, and she choked on a stone from a pill-box ring I had just got. It was a little bigger than an almond. I knew she had swallowed it but she appeared to be fine, but I knew something was not right. Dan took her to the local ER and at first they didn’t see anything then they lowered the placement of the X-ray and there lodged above her trachea was the stone. They decided it was best to have Dan come home and get me and us take her so she didn’t panic and get it completely stuck. We had to drive forty-five minutes to get to Dartmouth as the local hospital was not equipped to take it out safely. It took all night and in the morning the doctor came out, a little serious, and that stops your heart for a second, but they had to push it down into her tummy, because it kept falling out of the grip of the tool. While we had been waiting, I told God, this is not how He was going to take her. After all she had been through for her to choke on a pill box stone, NO WAY! Sometimes, prayer just comes out like that and that is okay. God understands and He loves us more for our honesty. She passed it out and I kept it as a token of God’s love and just for the humor of it.
This is just a part of Maddie’s life. She is a beauty inside and out. She is my little hero and she has taught me how to suffer with love. Although she gets anxious going for her appointments, like today, hiding under the Christmas tree so I couldn’t get her, as soon as it is over, she is laughing and waving at people making them smile. I love to see her give people who love her the biggest hugs. Maddie has fleeting moments where she is trying to understand why she is sick…it is often in the bathroom, and she doesn’t feel good. I usually sit on the edge of the tub, to keep her company. One night not too long ago, we were both tired but she was feeling sick and need to be on the potty. She was teary and said, “Why do I have to be sick and not anyone else?” I told Maddie that she was very special and that God had made her this way so she could be like Jesus and help people get to heaven. She beat her little fist on her knees and said,”I DON”T WANT THAT JOB!” It was so honest and real. She got very silly and goofy a few minutes later, then suddenly says to me,”Mommy, thank you for my tube.” I thought my heart would burst.
She is loved by her wonderful Daddy. Every night they have a tradition, after she gets changed on our bed, she says, “Princesses feet must never touch the ground” and Dan always carries her into bed, now with her Sister who is two and a half on his back. The baby who is ten months will soon be requesting the same treatment. Maddie’s older brothers are incredible and I am not just saying this. I am so proud of my boys, one is 9, the other is 8 and the youngest is 6. They really love their little sisters and have been so concerned for Maddie. They have teared up at seeing pictures of her when she was in Boston,and have willingly sacrificed their birthday parties because of Maddie being sick a lot or having a surgery. They might have a fleeting look of disappointment, but they quickly recover and understand. I have been so proud of them, but take their disappointment to heart, and promise that they’ll get their reward someday, because love is always rewarded. I told the boys about the party that would be for them too, their faces said it all, “Wow, a party for us and our friends!”
Dan and I have had an amazing support group, we have been surrounded by our wonderful, caring families, and good friends who stood by and share our sorrows, struggles and joys. They are often daily a phone call away and I have family and friends who would drop everything in a heartbeat to help us. We have been very blessed. Maddie had an OT who was faithful about coming to our house from the time that Maddie was three months until she was three and did incredible work with Maddie and was emotionally supportive to me. Maddie now has wonderful pre-school teachers in Jame’s House Pre-School- she gets multiple therapies, but mostly lots of love and cuddles. I am so grateful to these wonderful women for there support and understanding of Maddie’s conditions. I admire and respect these caregivers, because Maddie is not a job to them, but a beautiful human being…”
I have often taken a ride on the hope and prayers of family and friends, because there are some days that I have difficulty accepting that my little girl has to suffer so, but I know we are held in the arms of our Creator, our Comforter. To quote the Good Book, “Are not five sparrows sold for two cents? Yet not one of them is forgotten before God…Indeed, the very hairs of your head are all numbered. Do not fear; you are more valuable than many sparrows.”
Thank you for letting me share the Maddie story! (FROM STEVE…… Thank you also x)