Gastroesophageal reflux (GER, aka acid reflux or acid regurgitation) occurs when the opening to the stomach (lower oesophagal sphincter, LES) doesn’t close properly, causing food and digestive acid to rise up the oesophagus. This stomach acid irritates and inflames the oesophagus causing heartburn pain (esophagitis).
Persistent acid reflux is considered Gastroesophageal Reflux Disease (GERD), and it can eventually lead to more serious health problems including chronic esophagitis, causing pain and trouble swallowing. When gastroesophageal reflux results in persistent vomiting the vocal cords and small airways of the lung can become irritated leading to recurrent pneumonia, and breathing problems which can be mistaken for asthma.
Pediatric patients with gastroesophageal reflux have problems with irritability, poor feeding, slow growth, and respiratory trouble. For children with oesophagal birth defects, gastroesophageal reflux is common and may contribute to the formation of oesophagal narrowing or stricture, which makes swallowing difficult.
Diagnosis of gastroesophageal reflux
If gastroesophageal reflux is suspected, additional tests may be performed to test the severity of the condition:
-
Upper gastrointestinal (GI) contrast study
-
24-hour pH monitoring
-
Upper GI endoscopy (direct telescopic visualization)
-
Gastric emptying studies.
The type of studies performed depend on your child’s specific symptoms and condition. It is also important to determine if the GER is caused by some other condition, including esophageal or diaphragmatic birth defects.
Treatment of gastroesophageal reflux
Medical non-operative treatment
Initial treatment for GER is usually medical non-operative treatment. In infants, this includes upright positioning and thickened feedings with or without the addition of medicine that helps the stomach empty (Reglan®). Most infants respond to medical treatment and do not require a surgical procedure. H 2-blockers, such as cimetidine or ranitidine, also may improve the success of non-operative therapy. Proton-pump inhibitors (e.g., omeprazole, Prevacid®) have revolutionized medical therapy and are effective agents for the non-operative treatment of this disorder.
Surgical intervention may be considered if medical therapy was unsuccessful or if additional complications occur. With some esophageal birth defects, gastroesophageal reflux is a common problem and surgical intervention is often necessary.
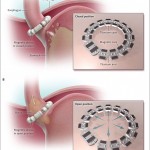
Fundoplication
The goal of a fundoplication is to prevent stomach contents from returning to the esophagus. This operation is accomplished by wrapping the upper portion of the stomach around the lower portion of the esophagus, tightening the outlet of the esophagus as it empties into the stomach. After a fundoplication, food and fluids can pass into the stomach but are prevented from returning to the esophagus and causing symptoms of esophageal reflux. A large skin incision may not be required. In most cases, a fundoplication can be performed by a pediatric surgeon using a small telescope and miniaturized instruments placed through three to four band-aid sized incisions on the abdomen.
Gastroesophageal reflux following repair of esophageal atresia and tracheoesophageal fistula.
OBJECTIVE:
This study represents the experience of a tertiary care center in the Kingdom of Saudi Arabia (KSA) on the long-term effect on the lungs of esophageal atresia (EA) and tracheoesophageal fistula repair (TEF), and to emphasize the magnitude of gastroesophageal reflux (GER) post-EA or post-TEF repair.
METHODS:
A retrospective review of all patients referred to the pulmonary clinic with EA/TEF or re-operative evaluations from the period 1993-2004 at King Faisal Specialist Hospital and Research Centre, Riyadh, KSA.
RESULTS:
Forty-one patients with confirmed EA/TEF (26 males and 15 females) were included in the study. Congenital anomalies were associated in 28 (68%). Gastroesophageal reflux developed in 39 (95%) of patients, 24 (59%) needed Nissen fundoplication. Esophageal stricture that required more than 3 dilations developed in 16 (46%) patients, esophageal dysmotility in 37 (90%) and hiatal hernia in 11 (27%). Pulmonary complications developed in >70% of the patients including persistent atelectasis, chronic aspiration pneumonia, asthma and chronic lung disease that required oxygen for more than one month. Tracheomalacia in 12 (29%) and bronchiectasis in 7 (17%). Eighty-eight percent of patients who were able to do pulmonary function test showed abnormal values of moderate obstructive and restrictive lung disease.
CONCLUSION:
Pulmonary complications cause significant and prolonged morbidities post EA/TEF repair. Gastroesophageal reflux is a common complication after EA/TEF repair and causes significant morbidity that needs a prolonged follow-up. Patients with GER may need Nissen fundal plication to improve respiratory problems.
www.ncbi.nlm.nih.gov/pubmed/15951870
Heartburn remedy?
An idea to help with Heartburn and GERD?
This was sent to me by a Parent, not everything works for all but this seemed to work for others, when I looked into it, before posting it on here. Plus the feedback from a large TEF support FB group was very positive. I can’t say this will work for you or your child only you will know, but it’s something, if not just an idea from other Parents.
(gastroesophageal reflux disease)
About heartburn causes: I don’t know what caused my episode. The Internet tells me that heartburn is commonly caused by an incompetence of the lower esophageal sphincter (LES), which is a kind of valve that connects the stomach with the esophagus. There is a long list of possible causes of this “incompetence” (eating too much, eating wrong, smoking, hiatus hernia, etc.). About the only thing that I was able to identify with was eating shortly before bedtime, and I have adjusted my habits accordingly. So far this seems to have helped, although I sometimes feel some acidity, which seems to occur when I make long breaks between meals.
First, I started taking Maalox ( a mixture of magnesium hydroxide and aluminum hydroxide) chewable tablets. I also considered Manti, but it is 50% more expensive (in Poland at least) and the only difference is that it also contains simethicone, which helps relieve excess gas. Maalox helped neutralize the acid, providing instant relief, but I found I had to take it at least once every 2 hours. That didn’t look like a good remedy to me.
Some obscure sites recommended eating Jonagold apples for heartburn and GERD (gastroesophageal reflux disease), which is a kind of chronic heartburn. The idea is that apples contain pectin, which neutralizes stomach acid, and Jonagolds have the most pectin. I could find no reputable sources recommending apples as a remedy, but I thought it was worth a try. What I found was that the apples worked well — they actually provided longer-lasting relief than Maalox.
Heartburn remedy: Ground flaxseed, also I am informed it could help with Constipation.
https://blog.szynalski.com/2009/05/14/heartburn-remedy-ground-flaxseed/

 How is the diagnosis of reflux made?
How is the diagnosis of reflux made?